Summary:
- BPA was studied as a pharmaceutical for synthetic estrogen in the 1930s
- One of the highest volume chemicals produced in the world, BPA is used in car parts, bulletproof windows, microwavable containers, and canned foods.
- BPA easily leaches from materials, especially after exposure to heat
- Research shows that BPA is linked to cancer development, particularly breast, prostate, ovarian, and endometrial cancers
- BPA negatively impacts fertility, growth, and development and significantly increases the risk of developing a host of chronic diseases
How would you react if I told you that 95% of the people in this world have a toxic chemical in their bloodstream? (Calafat et al., 2005) If you’ve ever turned on the news or shopped at a grocery store, you’ve likely heard about BPA. Bisphenol A is a chemical compound that is used to harden plastics. It can be found in every product imaginable, from food containers and water bottles to medical devices and DVDs. If a label doesn’t explicitly state “BPA-free,”— chances are, it has BPA. It is one of the highest volume chemicals produced in the world with over 6 billion pounds (2.7 billion kilograms) produced each year — that’s the equivalent of the weight in water of over 1,250 Olympic-sized swimming pools!
The History of BPA
The story of how this chemical was created and came to see such widespread use is both strange and shocking. It was first discovered in 1891 by Russian chemist Aleksandr Dianin. However, BPA wasn’t widely used or explored until the 1930s, when it was studied as a pharmaceutical for synthetic estrogen. Estrogen is a sex hormone produced in high amounts in females and low amounts in males. BPA has a remarkably similar chemical structure to estrogen (Figure 1). In fact, it’s so similar that our bodies can’t tell the difference between the two! It activates the same hormone receptors and behaves almost identically to innate estrogen (Gao et al., 2015).
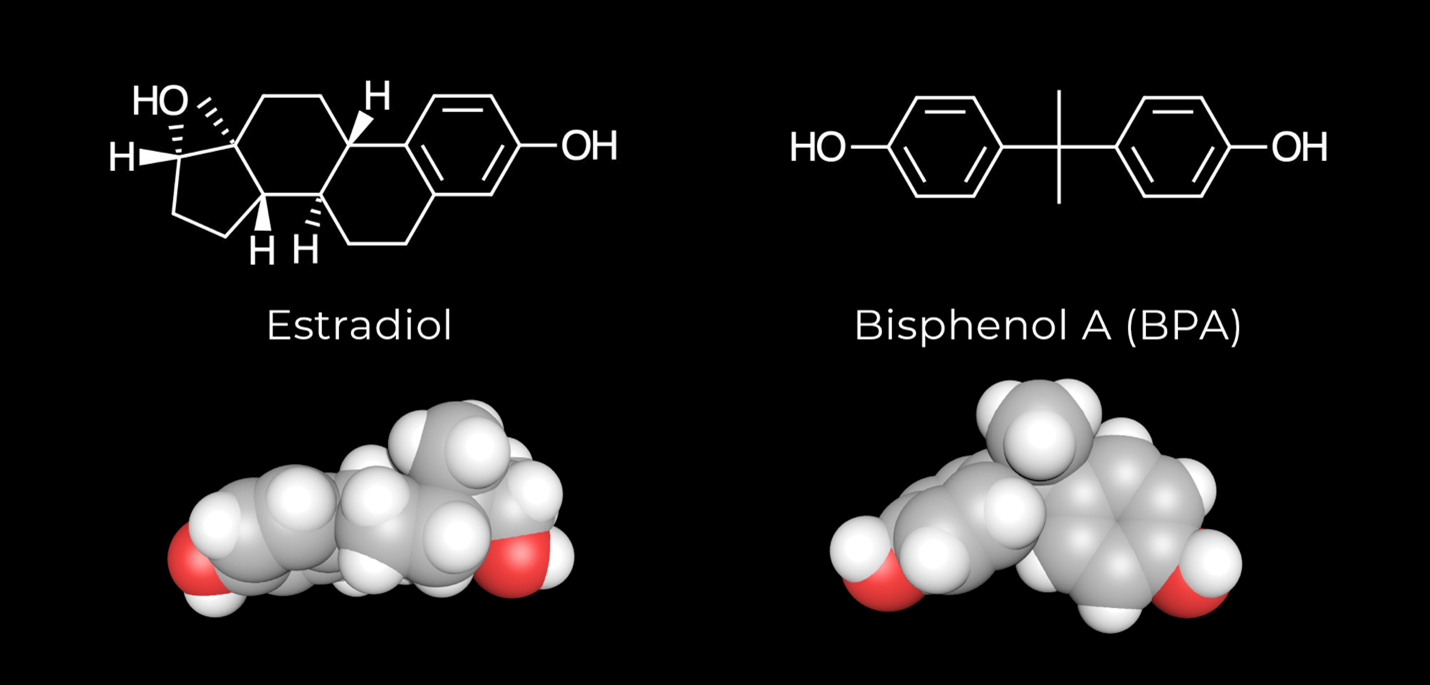
Figure 1. Comparison of 2D and 3D structures of estradiol (one of the forms of estrogen produced in the ovaries) (left) and BPA (right). The 3D structure shows the similarities in shapes and functionalities that allow BPA to mimic estrogen.
BPA would have gone on to be a pharmaceutical drug, but it took a backseat to a more potent chemical called diethylstilbestrol (DES). Interestingly, the FDA later took DES off the market after it was linked to reproductive cancers in babies born to mothers who were prescribed the drug. So how did BPA, a chemical once studied as a hormone-replacing pharmaceutical, come to see such widespread use in plastics?
Well, in the 1950s, scientists discovered that mixing BPA and another chemical created a hard, clear resin called polycarbonate. From a perspective of materials engineering, polycarbonate was a breakthrough discovery because of its durability and versatility. It could withstand high-impact collisions, which is how it became widespread in car parts, safety glasses, and bulletproof windows. It could also withstand exposure to heat, which is how it became widespread in microwavable food containers. It even extended the shelf life of canned foods when used as an internal liner (yet another reason why canned foods are unsafe to eat!).
But what wasn’t immediately apparent was that BPA easily leaches from these materials, especially when exposed to heat. This fact was discovered accidentally in the 1990s by Dr. David Feldman, a researcher at Stanford University. While experimenting with yeast, Dr. Feldman unexpectedly found BPA in his plastic laboratory flasks. He initially thought this chemical was a product of the biochemical reaction but, upon further research, he realized BPA was leaching from the laboratory flasks! This discovery brought to awareness the ubiquity of BPA in our everyday lives (Conger, 2008).
BPA and Its Connection to Cancer and Chronic Disease
Dr. Feldman’s revelation set off a chain of research about BPA, and it quickly became apparent how widespread the exposure was. Scientists soon discovered the presence of BPA in the vast majority of the population and concerns about its biological consequences started to rise, stimulating extensive research efforts.
The results were far from encouraging. Numerous animal studies began to show that both high and low levels of BPA interfered with the endocrine system and negatively impacted fertility, growth, and development. Researchers found that BPA exposure decreased the sperm count in mice (Adegoke et al., 2022), negatively impacted fetal development in frogs (Heimeier et al., 2009), and damaged sperm and eggs in fish (Zhang et al., 2018).
Further research mirrored these findings in humans and found adverse effects that extended far beyond fertility. BPA exposure has been linked to nearly every negative health outcome imaginable — from increased risk of developing diabetes, hypertension, and cardiovascular disease, to increased incidences of behavioral issues, aggression, and learning disabilities. It is also apparent that BPA can easily cross the placental barrier in humans, meaning unborn children are born with the chemical in their bodies (Liu et al., 2017). Figure 2 summarizes the multisystemic alterations induced by BPA (and a similar group of compounds called phthalates) through disruption of the endocrine system (Martínez-Ibarra et al., 2021).
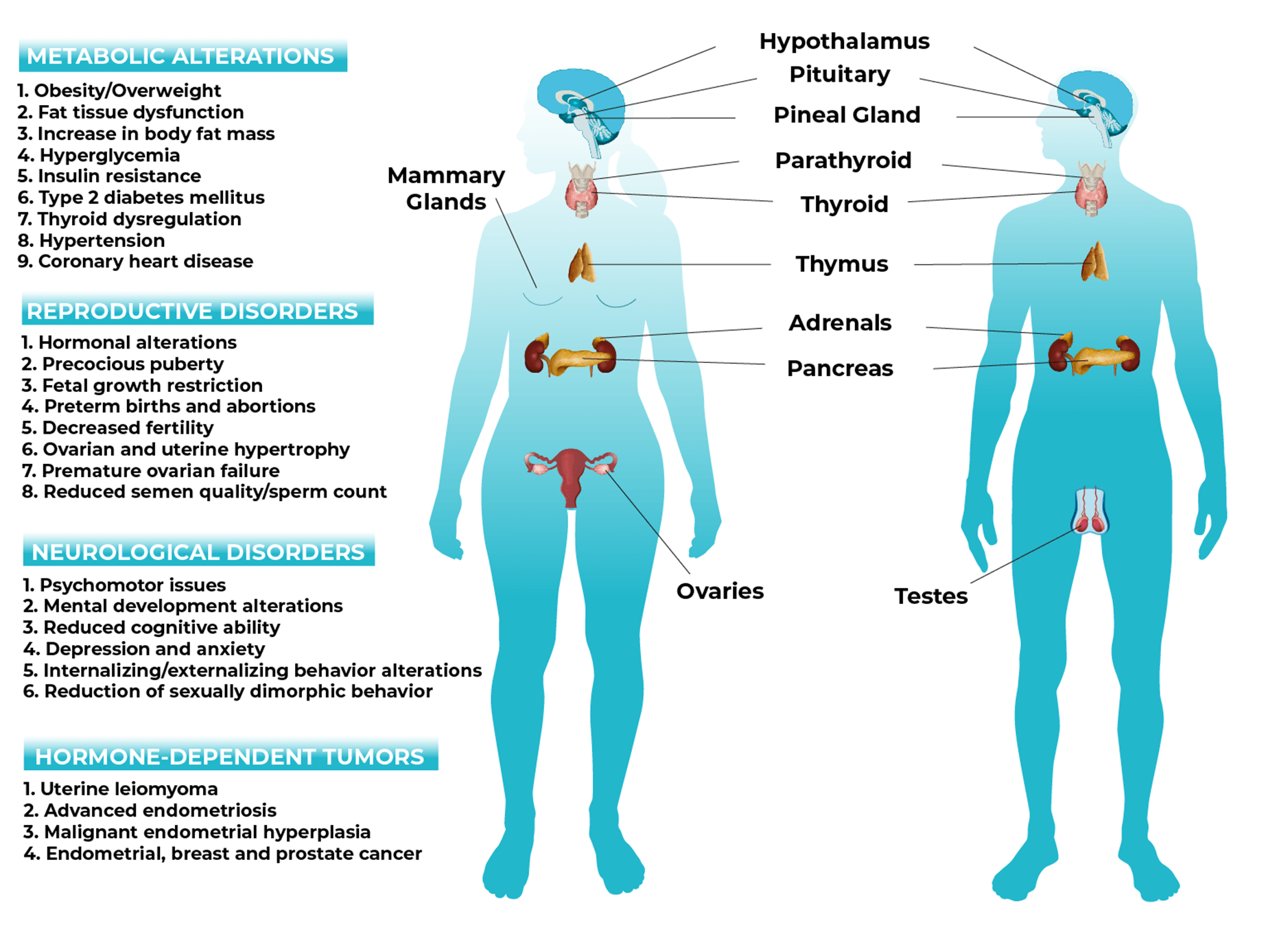
Figure 2. The endocrine disruptors, BPA and phthalates, can cause wide-ranging, multisystemic alterations in the human body (Martínez-Ibarra et al., 2021).
It is now well-established that BPA is also linked to cancer development, particularly hormone-related cancers such as breast, prostate, ovarian, and endometrial cancers (Cimmino et al., 2020). In a study analyzing the BPA concentrations in both cancerous and non-cancerous individuals, the levels of BPA in patients with cancer were significantly higher than in those without cancer (Keshavarz-Maleki et al., 2021). Another study showed that early-life exposure to BPA resulted in a higher susceptibility to developing breast and prostate cancers later in life and subsequently called for the classification of BPA as a carcinogen (Seachrist et al., 2016).
The Bureaucracy of BPA
Since the initial, accidental discovery that BPA was leaching into our foods, a vast body of research has linked BPA to adverse health outcomes. So, it begs the question—why hasn’t the FDA banned it?
To this day, despite research to the contrary, the FDA has maintained that BPA is safe. The FDA’s stance on BPA first became solidified in the 1970s when the first law was passed to regulate toxic chemicals. BPA, already widely in use at that time, was grandfathered in and presumed safe without any evidence to support that claim. As more troubling research emerged, the FDA doubled down by selectively citing a few research studies that found BPA to be safe.
But the studies used by the FDA to make this claim have a few issues. In 2000, the National Toxicology Program hosted an investigatory panel to thoroughly assess the pro-BPA research cited by the FDA. The panel found that many of the studies used to claim BPA were safe were full of errors and mistakes. One study, in particular, was quoted as being “misleading,” “flawed,” and “illogical.” Also, once re-analyzed, some of the studies that claimed “insignificant findings” were indeed significant and did show adverse effects of BPA! (National Toxicology Program, 2001)
These studies also had serious conflicts of interest. One of the pro-BPA studies by the Harvard Center for Risk Analysis (HCRA) was actually funded by the American Plastics Council (APC) (vom Saal & Hughes, 2005), and another study was conducted by a firm that was simultaneously working for two of the largest manufacturers of BPA (Timeline, 2008). Plastic companies have a vested interest in continuing to manufacture BPA, no matter the cost to public health. For this reason, BPA manufacturers funding BPA research should be met with suspicion.
As it currently stands, consumers and the scientific community are in a stalemate against BPA manufacturers and the FDA. But even though we are routinely and continuously exposed to BPA, there is cause for optimism. First, many companies have responded to public outcry and have taken it upon themselves to remove BPA from their products. While this doesn’t guarantee the safety of their products, it is certainly a step in the right direction. Also, by arming ourselves with knowledge, we can recognize, avoid, and detoxify from BPA. In the next blog article, we will discuss strategies for taking control of your exposure to this harmful chemical and living your healthiest life.
References
Adegoke, E. O., Rahman, M. S., Amjad, S., Pang, W. K., Ryu, D. Y., Park, Y. J., & Pang, M. G. (2022). Bisphenol A damages testicular junctional proteins transgenerationally in mice. Environ Pollut, 302, 119067.
Calafat, A. M., Kuklenyik, Z., Reidy, J. A., Caudill, S. P., Ekong, J., & Needham, L. L. (2005). Urinary concentrations of bisphenol A and 4-nonylphenol in a human reference population. Environ Health Perspect, 113(4), 391-395.
Cimmino, I., Fiory, F., Perruolo, G., Miele, C., Beguinot, F., Formisano, P., & Oriente, F. (2020). Potential Mechanisms of Bisphenol A (BPA) Contributing to Human Disease. Int J Mol Sci, 21(16).
Conger, K. (2008). 5 questions: Feldman on risk of bisphenol a in plastic bottles.
Gao, H., Yang, B. J., Li, N., Feng, L. M., Shi, X. Y., Zhao, W. H., & Liu, S. J. (2015). Bisphenol A and hormone-associated cancers: current progress and perspectives. Medicine (Baltimore), 94(1), e211.
Heimeier, R. A., Das, B., Buchholz, D. R., & Shi, Y. B. (2009). The xenoestrogen bisphenol A inhibits postembryonic vertebrate development by antagonizing gene regulation by thyroid hormone. Endocrinology, 150(6), 2964-2973.
Keshavarz-Maleki, R., Kaviani, A., Omranipour, R., Gholami, M., Khoshayand, M. R., Ostad, S. N., & Sabzevari, O. (2021). Bisphenol-A in biological samples of breast cancer mastectomy and mammoplasty patients and correlation with levels measured in urine and tissue. Sci Rep, 11(1), 18411.
Liu, J., Li, J., Wu, Y., Zhao, Y., Luo, F., Li, S., Yang, L., Moez, E. K., Dinu, I., & Martin, J. W. (2017). Bisphenol A Metabolites and Bisphenol S in Paired Maternal and Cord Serum. Environ Sci Technol, 51(4), 2456-2463.
Martínez-Ibarra, A., Martínez-Razo, L. D., MacDonald-Ramos, K., Morales-Pacheco, M., Vázquez-Martínez, E. R., López-López, M., Rodríguez Dorantes, M., & Cerbón, M. (2021). Multisystemic alterations in humans induced by bisphenol A and phthalates: Experimental, epidemiological and clinical studies reveal the need to change health policies. Environmental Pollution, 271, 116380.
Program, N. T. (2001). Endocrine Disruptors Low-Dose Peer Review Retrieved from https://ntp.niehs.nih.gov/ntp/pressctr/mtgs_wkshps/2000/lowdosepeerfinalrpt.pdf on Aug 3, 2022.
Seachrist, D. D., Bonk, K. W., Ho, S. M., Prins, G. S., Soto, A. M., & Keri, R. A. (2016). A review of the carcinogenic potential of bisphenol A. Reprod Toxicol, 59, 167-182.
Timeline: BPA from invention to phase-out. (2008). Environmental Working Group. Retrieved from https://www.ewg.org/research/timeline-bpa-invention-phase-out on Aug 3, 2022.
vom Saal, F. S., & Hughes, C. (2005). An extensive new literature concerning low-dose effects of bisphenol A shows the need for a new risk assessment. Environ Health Perspect, 113(8), 926-933.
Zhang, Y., Guan, Y., Zhang, T., Yuan, C., Liu, Y., & Wang, Z. (2018). Adult exposure to bisphenol A in rare minnow Gobiocypris rarus reduces sperm quality with disruption of testicular aquaporins. Chemosphere, 193, 365-375.




Sorry where’s the how to detox from it you linked on Instagram??
The wrong graphic was posted at first, but did have the correct caption, which discussed this article. It was corrected shortly after being posted. Sorry for the confusion. That article will be coming soon so stay tuned!
Highly informative Clinical informatics, this truth about BPA and it’s carcinogenicity should be widely publicized, most especially those in the Integrative Medicine field as allopthic clinicians has decided to play along the companies producing products with Bisphenol A and not informing patients to steer clear any product containing BPA. My teacher said that Integrative Medicine practitioners should educate all and sundry Viz: Medical doctors, nurses, market women, mechanics, engineers etc on the medicine for today, tomorrow and the future – Integrative Medicine – because it has come to cure the ills and bridge that gap with other forms of medical practice.
We are so happy to hear you enjoyed the article!